Graham W Warren1, Anurag K Singh2
1 Department of Radiation Oncology; Cell and Molecular Pharmacology and Experimental Therapeutics, Medical University of South Carolina, Charleston, SC, USA and Roswell Park Cancer Institute, Buffalo, NY, USA
2 Department of Radiation Medicine, Medical University of South Carolina, Charleston, SC, USA and Roswell Park Cancer Institute, Buffalo, NY, USA
| Date of Submission | 23-Jul-2012 |
| Date of Acceptance | 13-Dec-2012 |
| Date of Web Publication | 31-Jan-2013 |
Correspondence Address:
Graham W Warren
Department of Radiation Oncology; Cell and Molecular Pharmacology and Experimental Therapeutics, Medical University of South Carolina, Charleston, SC, USA and Roswell Park Cancer Institute, Buffalo, NY
USA
Source of Support: None, Conflict of Interest: None
DOI: 10.4103/1477-3163.106680
Abstract
Tobacco use in cancer patients is associated with increased cancer treatment failure and decreased survival. Nicotine is one of over 7,000 compounds in tobacco smoke and nicotine is the principal chemical associated with addiction. The purpose of this article is to review the tumor promoting activities of nicotine. Nicotine and its metabolites can promote tumor growth through increased proliferation, angiogenesis, migration, invasion, epithelial to mesenchymal transition, and stimulation of autocrine loops associated with tumor growth. Furthermore, nicotine can decrease the biologic effectiveness of conventional cancer treatments such as chemotherapy and radiotherapy. Common mechanisms appear to involve activation of nicotinic acetylcholine receptors and beta-adrenergic receptors leading to downstream activation of parallel signal transduction pathways that facilitate tumor progression and resistance to treatment. Data suggest that nicotine may be an important mechanism by which tobacco promotes tumor development, progression, and resistance to cancer treatment.
Keywords: Cancer, lung, nicotine, smoking, tobacco
| How to cite this article: Warren GW, Singh AK. Nicotine and lung cancer. J Carcinog 2013;12:1 |
| How to cite this URL: Warren GW, Singh AK. Nicotine and lung cancer. J Carcinog [serial online] 2013 [cited 2021 Oct 25];12:1. Available from: https://carcinogenesis.com/text.asp?2013/12/1/1/106680 |
Background
Tobacco use is the largest preventable cause of cancer with an estimated 30% of all cancer deaths attributed to tobacco use. [1 ],[2],[3],[4] Cigarette smoke is the predominant form of tobacco consumption consisting of approximately 95% of tobacco use. There are an estimated 7,000 compounds in cigarette smoke including at least 60 known carcinogens. [4] Though there is tremendous literature supporting the role of tobacco in carcinogenesis, there are proportionately few studies that report on the effects of tobacco on cancer treatment outcomes. Several studies demonstrate that tobacco decreases survival, decreases quality of life, impairs wound healing, increases recurrence, and decreases survival in patients with well-established tobacco-related cancers such as head and neck or lung cancer. [5],[6],[7],[8],[9],[10],[11] In traditionally non-tobacco-related cancers, tobacco use is also associated with a more advanced stage at diagnosis, younger age at cancer presentation, decreased compliance to cancer treatment, decreased quality of life, increased risk of treatment toxicity, increased risk of developing second primary cancers, increased surgical risk, increased recurrence, and increased risk of cancer-related and non-cancer-related mortality. [12 ],[13],[14],[15],[16],[17],[18],[19],[20],[21],[22],[23],[24],[25],[26],[27],[28],[29],[30],[31],[32],[33],[34],[35],[36],[37] Importantly, tobacco use may dominate overall mortality in some non-tobacco-related cancers (such as prostate cancer) due to significantly increased risks of cardiovascular mortality. [14],[15],[38] There are limited data evaluating the effects of smoking cessation on outcome, but data suggest that tobacco cessation improves outcomes in cancer patients. [39],[40],[41] In more structured evaluations, patients who did not smoke a median of 32 days after completion of radiotherapy have improved survival as compared with patients who smoked during radiotherapy. [42] Collectively, these data support tobacco assessment and cessation as important to improve cancer treatment outcomes.
With the given adverse effects of tobacco on health, recommendations for tobacco cessation are supported by several national cancer organizations including the American Society for Clinical Oncology, [43] American Association for Cancer Research, [44] and National Comprehensive Care Network. [45] Public Health Service Guidelines are the mainstay for tobacco cessation that recommends providing behavioral counseling and pharmacotherapy to help support effective tobacco cessation. [46] Nicotine, varenicline (Chantix), and bupropion (Zyban) are the most commonly used and well-supported pharmacotherapies used in tobacco cessation. Nicotine is a component of tobacco and cigarette smoke that is the primary component associated with addiction. [2],[46],[47] Nicotine is a systemically available agent that exerts many of its biological effects through the binding and activation of nicotinic acetylcholine receptors (nAChRs) that are known to be expressed on both normal and cancerous tissues. [48],[49],[50],[51] Though once associated primarily with neuronal signaling, nAChRs are increasingly implicated in the pathogenesis and progression of cancer. [52],[53] The purpose of this review is to introduce the cellular and physiological activities of nicotine as related to the biological development, progression, and treatment of lung cancer.
Nicotine Chemistry And Metabolisma
Nicotine is a product of tobacco that undergoes several pathways of chemical conversion and metabolism. [48],[49] During the tobacco curing and smoking process, nicotine can be converted to 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone (NNK), 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanol, and N’- nitrosonornicotine (NNN) through nitrosation. After entering the body, nicotine is rapidly absorbed and distributed throughout the body. Approximately 75% of nicotine is metabolized to cotinine primarily by cytochrome P450 (CYP) 2A6, CYP2B6, and aldehyde oxidase. Further metabolism of cotinine involves additional hydroxylation primarily to 3-OH cotinine, glucuronidation, and excretion primarily in urine. Approximately 50-60% of nicotine is metabolized and excreted as glucuronidated 3-OH cotinine. The remaining nicotine can be converted to other metabolites such as nicotine-N-oxide. Glucuronidated nicotine and its metabolites are also excreted in the urine. [48],[49] Nicotine and its principal metabolites involved in tumor promotion are shown in [Figure 1].
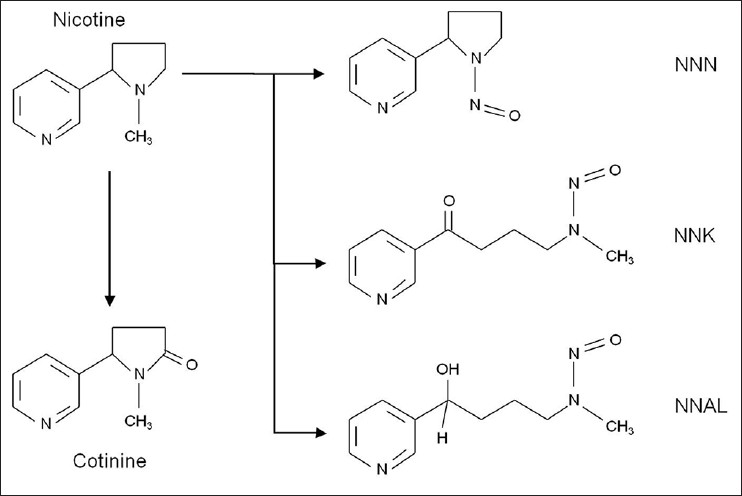 |
Figure 1: Nicotine and metabolites associated with tumor promotion [NNAL: 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanol, NNK: 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone, NNN: N’-nitrosonornicotine, NNO: Nicotine-N-oxide] Click here to view |
Tumorigenesis
Nicotine alone is generally accepted as a tumor promoter, but not a tumor initiator in carcinogenesis. However, NNK is a well-established initiating carcinogen that can lead to tumor development. NNK tumorigenesis is enhanced with beta-adrenergic receptor (β-AdrR) stimulation and reduced with inhibition of β-AdrRs. [54] Similar studies demonstrate that inhibition of 5-lipoxygenase or cyclooxygenase-2 (COX-2) decreases tumorigenesis by NNK. [55],[56] Beyond initiation, NNK can promote tumor development through activation of nAChRs and β-AdrRs leading to increased proliferation. [57] NNK or NNN can increase transformation of immortalized cells, though these effects of NNK appear to be related primarily to activation of the α7nAChR, whereas the effects of NNN may be preferentially modulated through the α3nAChR. [58] The potential importance of nAChRs in regulating tumor growth is demonstrated by recent data showing that inhibition of nAChRs in vivo decreases tumor growth by approximately 90%. [59] In this latter study, preferential inhibition of the α7nAChR results in significant apoptosis in tumor xenografts associated with significant decreases in angiogenesis.
Nicotine and its metabolites may facilitate tumorigenesis by other carcinogens. Nicotine administration in human bronchial epithelial cells significantly upregulates several genes particularly associated with activation of mitogen activated protein kinase (MAPK). [60] Nicotine increases methylation of the fragile histidine triad (FHIT) gene resulting in decreased FHIT and increased deoxyribonucleic acid (DNA) methyltransferase (DNMT) 3a expression. [61] Notably, removal of nicotine restores normal methylation patterns and expression suggesting the effect of nicotine is reversible. Cotinine may also increase the tumor forming effects of NNK. [62] However, other studies suggest that nicotine has no appreciable effects on tumor number, size, or metastasis by NNK. [63],[64]
Recent evidence suggests that variations in the tumor-promoting effects of nicotine are mediated in part by p53 expression. In cells without p53 function, nicotine has a more pronounced pro-survival effect in cells treated with cytotoxic agents or serum starvation. [65],[66] Translocation of nuclear factor kappa-B (NFκB) to the nucleus in cells without functional p53 also occurs at lower doses of nicotine, thereby promoting tumor growth. [67] Data suggest that nicotine decreases G1 arrest following DNA damage by several cytotoxic agents, thereby promoting cellular transformation and tumor formation. [65],[68] A more pronounced effect of nicotine in cells without functional p53 supports a cellular alteration in cell cycle checkpoint, thereby promoting tumorigenesis through dysregulation of proliferation, DNA repair, and apoptosis. However, the removal of nicotine from combustible products does not appear to reduce DNA damage [69] and nicotine replacement therapy has no appreciable effect on the development of lung cancer in clinical cohorts. [70]
Proliferation
Nicotine and activation of nAChRs appear to be important in the proliferative effects of cigarette smoke. In C57BL/6J mice engrafted with Lewis lung cancer cells, smoke increases cotinine levels and increases tumor size, weight, capillary density, and circulating serum vascular endothelial growth factor (VEGF). [71] Inhibition of nAChRs with mecamylamine partially prevents the effects of second-hand smoke on tumor growth and VEGF levels. Further examination of nAChRs suggests that they are important in tumor proliferation. Evaluation of small-cell lung cancer (SCLC) cell lines demonstrates that acetylcholine increases proliferation and SCLC has broad nAChR subunit expression as well as the ability to synthesize, secrete, and metabolize acetylcholine. [72] Treatment of H69 SCLC cells with nicotinic agonists (nicotine or cytisine) increases proliferation through activation of nAChRs, [73] but inhibition of muscarinic AChRs does not prevent the proliferative effects of nicotine. [74] Nicotine increases proliferation of SCLC cells in a manner prevented with inhibition of the α7nAChR, but higher doses of nicotine result in the loss of proliferative stimulus. [75] In this study, nicotine does not appear to increase proliferation in non-malignant cells. The proliferative effects of nicotine and its metabolites may vary by cell type. Studies in BEP2D bronchial epithelial cells demonstrate broad nAChR expression and increased proliferation with NNK or NNN through activation of nAChRs. [76] Nicotine or NNK increases proliferation in neuroendocrine cells (H727) with no effect in type II alveolar cells; however although NNK increases Clara cell proliferation, nicotine has no effect. [77]
Data also suggest that nicotine and other agonists of the nAChR can stimulate an autocrine loop to promote proliferation. Nicotine or cytosine (a nAChR agonist) increases proliferation and serotonin production through activation of nAChRs; however, serotonin increases proliferation independently of nAChR. [78] Furthermore, serotonergic-induced proliferation is not enhanced in the presence of nicotine. [79] Nicotine can increase proliferation or secretion of noradrenaline and adrenaline in pancreatic cancer cells through activation of nAChR and β-AdrR. [80] Collectively, these data suggest that nicotine and its metabolites increase proliferation of malignant and non-malignant cells through modulation of nAChRs, β-AdrRs, and potential activation of proliferative autocrine loops.
Nicotine and its metabolites increase proliferation through activation of several downstream pathways. Nicotine increases proliferation associated with increased activation of MAPK and DNA synthesis in a α7nAChR-dependent manner. [81] Further examination in vivo suggests that nicotine activates MAPK kinase (MEK) leading to downstream activation of extracellular signal related kinase (ERK) 1/2, COX-2 expression, prostaglandin production, VEGF expression, and proliferation. [82],[83] Nicotine-induced proliferation in colon cancer cells is partially and synergistically prevented with inhibition of epidermal growth factor receptor tyrosine kinase (EGFR-TK) and Src. [84] Similar activation of proliferation through Src, cyclin dependent kinase (CDK), Raf-1, beta-arrestin, and EGFR-TK is also observed in lung cancer cells and endothelial cells [66],[85] The molecular pathways activated by nicotine are presented in [Figure 2].
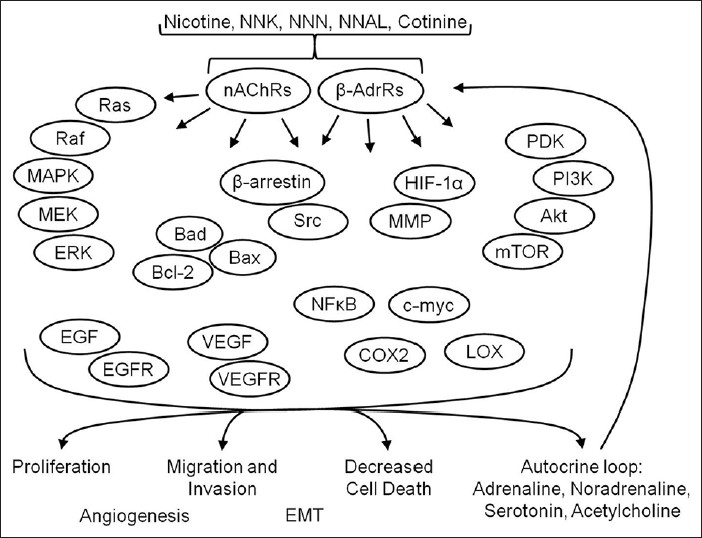 |
Figure 2: Principal mechanisms of tumor promotion by nicotine and its metabolites. Nicotine and its metabolites primarily promote tumor growth, angiogenesis, migration, invasion, epithelial to mesenchymal transition, and resistance to cancer treatment. Shown are downstream proteins and signal transduction pathways associated with activation of b -AdrRs and nAChRs by nicotine and its metabolites Click here to view |
NNK and NNN are also activators of proliferation and tumor promotion through activation of the nAChRs and β-AdrRs. Whereas the effects of NNK preferentially modulate α7nAChRs, NNN may preferentially modulate proliferation through α3nAChRs. [57],[58],[86],[87] In non-small-cell lung cancer and SCLC lines, nicotine or NNK activates nAChRs and Akt leading to increased Cyclin D1 expression and proliferation. [88] Notably, NNK induces proliferation at markedly lower doses than proliferation induced by nicotine. Proliferation induced by NNK in immortalized human pancreatic cells appears to be dependent upon β-AdrRs, adenylyl cyclase, ERK, and EGFR-TK. [89] In SCLC, NNK-induced proliferation appears to involve activation of the α7nAChRs, MEK, protein kinase C (PKC), and c-myc. [90] The common downstream signals following nAChR or β-AdrR activation appear to suggest that activation of MAPK, MEK, and ERK 1/2 are important in the proliferative effects of nicotine and its metabolites.
Angiogenesis
Several studies demonstrate that nicotine increases angiogenesis in tumor models as well as with endothelial cells in models of limb ischemia. [52] Nicotine increases proliferation and decreases hypoxia-induced apoptosis in endothelial cells. [91] Further examination demonstrates that nicotine increases tumor growth associated with increased VEGF secretion in mice inoculated with Lewis lung cancer cells. [91] Broad nAChR expression is noted in endothelial cells and nicotine or hypoxia increases expression of the α7nAChR. [92] In this latter study, inhibition of the nAChR prevents endothelial network formation and agonists of the α7nAChR increase endothelial network formation with concomitant increases in VEGF production. The effects of nicotine or nAChR agonists are prevented with inhibition of MAPK, MEK, phosphatidylinositol-3-kinase (PI3K), or NFκB. Notably, angiogenesis is reduced in α7nAChR knockout mice and non-specific inhibition of nAChRs decreases vascular diameter without decreasing the number of vascular collaterals. [92] Separate studies also demonstrate that nicotine-induced angiogenesis can be prevented with inhibition of the α7nAChR in mice containing SCLC xenografts. [93] Data also suggest that inhibition of COX-2 may prevent the angiogenic effects of nicotine. [82] NNK also increases angiogenesis and VEGF production. [94] and co-administration of nicotine with estradiol results in synergistic increase in tumor growth, angiogenesis, and VEGF production. [95] The diverse pathways and effects of nicotine on angiogenesis are extensively reviewed by others discussing the role of the α7nAChR leading to activation of β-arrestin, Src, Raf-1, and Rb. [96]
Migration, invasion, and epithelial to mesenchymal transition
One of the most deadly consequences of lung cancer is the inherent ability for lung cancer to invade and metastasize. Data demonstrate that nicotine and activation of nAChRs can promote migration, invasion, and epithelial to mesenchymal transition (EMT). Repeated exposure of SCLC to nicotine increases collagen breakdown and transmigration in conjunction with increased tumor growth, vascularity, and resistance to chemotherapy. [69] Nicotine increases migration and invasion of lung cancer cells through activation of the α7nAChR, c-Src, and PKCiota. [97] The critical role of the α7nAChR on nicotine-induced migration or invasion is also observed in other cancer cells. [98],[99],[100],[101] Recent data suggest that MUC4 and ID1 (inhibitor of differentiation-1) are important to the angiogenic effects of nicotine and/or cigarette smoke [98],[102] NNK can also increase migration and invasion of lung cancer cells through activation of MEK and downstream activation of calpains. [103] The effects of NNK also appear to be dependent upon the α7nAChR. [104] Although nicotine increases the migration and invasion of cancer cells, the opposite appears to occur with immune cells. In vivo, nicotine administration appears to decrease migration of leukocytes and decreases chemotaxis of peripheral blood mononuclear cells. [105]
Nicotine can also increase malignancy through EMT. In A549 lung cancer cells, nicotine increases proliferation, migration, invasion, and EMT. [106] Many of the effects of nicotine are prevented through inhibition of the α7nAChR or Src and similar results are observed in breast cancer cells. In a separate study, nicotine increases aldehyde dehydrogenase expressing cells (a marker for EMT) in breast cancer through activation of the α7nAChR. [107]
Cell death and apoptosis
Beyond simply promoting tumor growth, nicotine also decreases the effectiveness of cancer treatment. Numerous studies demonstrate that nicotine decreases the effectiveness of chemotherapy through decreased apoptosis. The anti-apoptotic effects of nicotine are observed in multiple cell lines treated with multiple chemotherapeutic agents. [108] Activation of PI3K leading to increased XIAP, survivin, and recruitment of E2F1 to the genome appears to be important for the pro-survival effects of nicotine. [108] Nicotine decreases apoptosis in lung cancer cells through inactivation of PP2A, Bax phosphorylation, and decreased cytochrome c release. [109] Similar observations are noted with NNK through phosphorylation of Bcl-2 at Ser70. [90] Several studies suggest that activation of PI3K, Akt, and NFκB are critical to the pro-survival effects of nicotine on chemotherapy. [88],[110],[111],[112] Nicotine also decreases the cytotoxicity of several treatments (cisplatin, UV irradiation, and gamma irradiation) through decreased apoptosis, but not through changes in DNA repair or adduct formation. [113] Interestingly, acute nicotine or NNK decreases apoptosis from cisplatin, but the effects of NNK are much more potent than nicotine. However, although long-term nicotine or nicotine combined with NNK continued to confer resistance to cisplatin, long-term NNK had no significant effect on apoptosis. [114]
Activation of β-AdrRs is also implicated in the pro-survival effects of nicotine and its metabolites. In A549 lung cancer cells, NNK increases survival following chemotherapy through activation of β-AdrRs, Src, PKCiota, and phosphorylation of Bad. [115] However, in SCLC, NNK activates Bcl-2 leading to decreased apoptosis through activation of the α7nAChR. [90] Nicotine-induced phosphorylation of Bax and associated decrease in cisplatin-induced apoptosis are prevented with inhibition of the β-AdrR, but not with inhibition of the α7nAChR. [111] These apparent conflicting results between cell lines may potentially be explained by differences in receptor expression between cell lines coupled by similar parallel downstream pathways after activation of β-AdrRs or nAChRs.
Recent data demonstrate that nicotine decreases the effectiveness of radiotherapy (RT) and/or chemoradiotherapy (CRT) in vivo. [116] In vitro, nicotine increased survival in H460 and A549 lung cancer cells treated with RT through activation of PI3K. In vivo, nicotine decreases the effectiveness of RT and CRT on lung cancer xenografts. Importantly, the effects of nicotine only during RT/CRT appear to be identical to the effects of nicotine during and following RT/CRT suggesting that nicotine exposure specifically during the time of RT/CRT is the critical determinant of therapeutic response. Additional examination demonstrates that nicotine increases hypoxia inducible factor 1-alpha (HIF-1α) in a PI3K-dependent manner in vitro and nicotine specifically increases HIF-1α expression in a specific morphological pattern without altering pathological markers of hypoxia in vivo. [116] Collectively, this study suggests that nicotine decreases therapeutic response during treatment through alterations in protein expression in specific subpopulations of tumor cells.
Conclusions
Data suggest that nicotine may have a broad spectrum of tumor-promoting activities in lung cancer. Nicotine and its metabolites increase proliferation, migration, invasion, EMT, and angiogenesis with a concomitant decrease in sensitivity to chemotherapy and/or radiotherapy [Figure 2]. The effects of nicotine occur through activation of nAChRs and β-AdrRs leading to common downstream activation of Src, Ras-Raf-MAPK-MEK-ERK pathways, and PI3K-Akt pathways that further drive several parallel oncogenic pathways. Nicotine and its metabolites can promote tumor progression through modulation of oncogenic signals in both cancerous and non-cancerous tissues. Substantial work is required to definitively test the effects of nicotine on clinical outcomes in cancer patients, but current data suggest that nicotine is not a benign substance in cancer progression and therapy.
References
| 1. | Doll R, Peto R. The Causes of Cancer. New York: Oxford Press; 1981. p. 1-144.  |
| 2. | U.S. Department of Health and Human Services: Reducing the Health Consequences of Smoking: 25 Years of Progress. A Report of the Surgeon General. Rockville, MD: U.S. Department of Health and Human Services, Public Health Service, Centers for Disease Control, Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health. DHHS Publication No. CDC (89-8411), 1989.  |
| 3. | Secretan B, Straif K, Baan R, Grosse Y, El Ghissassi F, Bouvard V, et al. A review of human carcinogens – Part E: Tobacco, areca nut, alcohol, coal smoke, and salted fish. Lancet Oncol 2009;10:1033-4.  |
| 4. | U.S. Department of Health and Human Services. How tobacco smoke causes disease: The Biology and Behavioral basis for smoking-attributable disease: A report of the surgeon general. Atlanta, GA: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health, 2010.  |
| 5. | Rades D, Setter C, Schild SE, Dunst J. Effect of smoking during radiotherapy, respiratory insufficiency, and hemoglobin levels on outcome in patients irradiated for non-small-cell lung cancer. Int J Radiat Oncol Biol Phys 2008;71:1134-42.  [PUBMED] |
| 6. | Tammemagi CM, Neslund-Dudas C, Simoff M, Kvale P. Smoking and lung cancer survival: The role of comorbidity and treatment. Chest 2004;125:27-37.  [PUBMED] |
| 7. | Stevens MH, Gardner JW, Parkin JL, Johnson LP. Head and neck cancer survival and life-style change. Arch Otolaryngol 1983;109:746-9.  [PUBMED] |
| 8. | Phillips B, Marshall ME, Brown S, Thompson JS. Effect of smoking on human natural killer cell activity. Cancer 1985;56:2789-92.  [PUBMED] |
| 9. | Videtic GM, Stitt LW, Dar AR, Kocha WI, Tomiak AT, Truong PT, et al. Continued cigarette smoking by patients receiving concurrent chemoradiotherapy for limited-stage small-cell lung cancer is associated with decreased survival. J Clin Oncol 2003;21:1544-9.  [PUBMED] |
| 10. | Marshak G, Brenner B, Shvero J, Shapira J, Ophir D, Hochman I, et al. Prognostic factors for local control of early glottic cancer: The Rabin Medical Center retrospective study on 207 patients. Int J Radiat Oncol Biol Phys 1999;43:1009-13.  [PUBMED] |
| 11. | Marin VP, Pytynia KB, Langstein HN, Dahlstrom KR, Wei Q, Sturgis EM. Serum cotinine concentration and wound complications in head and neck reconstruction. Plast Reconstr Surg 2008;121:451-7.  [PUBMED] |
| 12. | Abramowitz MC, Li T, Morrow M, Anderson PR, Bleicher RJ, Goldstein LJ, et al. History of smoking is associated with younger age at diagnosis of breast cancer. Breast J 2010;16:344-9.  [PUBMED] |
| 13. | Roxburgh CS, Platt JJ, Leitch EF, Kinsella J, Horgan PG, McMillan DC. Relationship between preoperative comorbidity, systemic inflammatory response, and survival in patients undergoing curative resection for colorectal cancer. Ann Surg Oncol 2011;18:997-1005.  [PUBMED] |
| 14. | Zu K, Giovannucci E. Smoking and aggressive prostate cancer: A review of the epidemiologic evidence. Cancer Causes Control 2009;20:1799-810.  [PUBMED] |
| 15. | Joshu CE, Mondul AM, Meinhold CL, Humphreys EB, Han M, Walsh PC, et al. Cigarette smoking and prostate cancer recurrence after prostatectomy. J Natl Cancer Inst 2011;103:835-8.  [PUBMED] |
| 16. | Vaporciyan AA, Merriman KW, Ece F, Roth JA, Smythe WR, Swisher SG, et al. Incidence of major pulmonary morbidity after pneumonectomy: Association with timing of smoking cessation. Ann Thorac Surg 2002;73:420-5.  [PUBMED] |
| 17. | Møller AM, Pedersen T, Villebro N, Schnaberich A, Haas M, Tønnesen R. A study of the impact of long-term tobacco smoking on postoperative intensive care admission. Anaesthesia 2003;58:55-9.  |
| 18. | Fujisawa T, Iizasa T, Saitoh Y, Sekine Y, Motohashi S, Yasukawa T, et al. Smoking before surgery predicts poor long-term survival in patients with stage I non-small-cell lung carcinomas. J Clin Oncol 1999;17:2086-91.  |
| 19. | Goodwin SJ, McCarthy CM, Pusic AL, Bui D, Howard M, Disa JJ, et al. Complications in smokers after postmastectomy tissue expander/implant breast reconstruction. Ann Plast Surg 2005;55:16-19.  |
| 20. | Richards CH, Platt JJ, Anderson JH, McKee RF, Horgan PG, McMillan DC. The impact of perioperative risk, tumor pathology and surgical complications on disease recurrence following potentially curative resection of colorectal cancer. Ann Surg 2011;254:83-9.  |
| 21. | Chang DW, Reece GP, Wang B, Robb GL, Miller MJ, Evans GR, et al. Effect of smoking on complications in patients undergoing free TRAM flap breast reconstruction. Plast Reconstr Surg 2000;105:2374-80.  |
| 22. | Lin JH, Zhang SM, Manson JE. Predicting adherence to tamoxifen for breast cancer adjuvant therapy and prevention. Cancer Prev Res (Phila) 2011;4:1360-5.  |
| 23. | Komenaka IK, Hsu CH, Martinez ME, Bouton ME, Low BG, Salganick JA, et al. Preoperative chemotherapy for operable breast cancer is associated with better compliance with adjuvant therapy in matched stage II and IIIA patients. Oncologist 2011;16:742-51.  |
| 24. | Land SR, Cronin WM, Wickerham DL, Costantino JP, Christian NJ, Klein WM, et al. Cigarette smoking, obesity, physical activity, and alcohol use as predictors of chemoprevention adherence in the National Surgical Adjuvant Breast and Bowel Project P-1 Breast Cancer Prevention Trial. Cancer Prev Res (Phila) 2011;4:1393-400.  |
| 25. | Alsadius D, Hedelin M, Johansson KA, Pettersson N, Wilderäng U, Lundstedt D, et al. Tobacco smoking and long-lasting symptoms from the bowel and the anal-sphincter region after radiotherapy for prostate cancer. Radiother Oncol 2011;101:495-501.  |
| 26. | Marks DI, Ballen K, Logan BR, Wang Z, Sobocinski KA, Bacigalupo A, et al. The effect of smoking on allogeneic transplant outcomes. Biol Blood Marrow Transplant 2009;15:1277-87.  |
| 27. | Eifel PJ, Jhingran A, Bodurka DC, Levenback C, Thames H. Correlation of smoking history and other patient characteristics with major complications of pelvic radiation therapy for cervical cancer. J Clin Oncol 2002;20:3651-7.  |
| 28. | Ford MB, Sigurdson AJ, Petrulis ES, Ng CS, Kemp B, Cooksley C, et al. Effects of smoking and radiotherapy on lung carcinoma in breast carcinoma survivors. Cancer 2003;98:1457-64.  |
| 29. | Kaufman EL, Jacobson JS, Hershman DL, Desai M, Neugut AI. Effect of breast cancer radiotherapy and cigarette smoking on risk of second primary lung cancer. J Clin Oncol 2008;26:392-8.  |
| 30. | Boorjian S, Cowan JE, Konety BR, DuChane J, Tewari A, Carroll PR, et al. Bladder cancer incidence and risk factors in men with prostate cancer: Results from Cancer of the Prostate Strategic Urologic Research Endeavor. J Urol 2007;177:883-7.  |
| 31. | Waggoner SE, Darcy KM, Fuhrman B, Parham G, Lucci J 3 rd , Monk BJ, et al. Association between cigarette smoking and prognosis in locally advanced cervical carcinoma treated with chemoradiation: A Gynecologic Oncology Group study. Gynecol Oncol 2006;103:853-8.  |
| 32. | Jang S, Prizment A, Haddad T, Robien K, Lazovich D. Smoking and quality of life among female survivors of breast, colorectal and endometrial cancers in a prospective cohort study. J Cancer Surviv 2011;5:115-22.  |
| 33. | Hawkes AL, Lynch BM, Owen N, Aitken JF. Lifestyle factors associated concurrently and prospectively with co-morbid cardiovascular disease in a population-based cohort of colorectal cancer survivors. Eur J Cancer 2011;47:267-76.  |
| 34. | Hooning MJ, Botma A, Aleman BM, Baaijens MH, Bartelink H, Klijn JG, et al. Long-term risk of cardiovascular disease in 10-year survivors of breast cancer. J Natl Cancer Inst 2007;99:365-75.  |
| 35. | Jagsi R, Griffith KA, Koelling T, Roberts R, Pierce LJ. Rates of myocardial infarction and coronary artery disease and risk factors in patients treated with radiation therapy for early-stage breast cancer. Cancer 2007;109:650-7.  |
| 36. | Yu GP, Ostroff JS, Zhang ZF, Tang J, Schantz SP. Smoking history and cancer patient survival: A hospital cancer registry study. Cancer Detect Prev 1997;21:497-509.  |
| 37. | Warren GW, Kasza KA, Reid ME, Cummings KM, Marshall JR. Smoking at diagnosis and survival in cancer patients. Int J Cancer 2013;132:401-10.  |
| 38. | Bittner N, Merrick GS, Galbreath RW, Butler WM, Wallner KE, Allen ZA, et al. Primary causes of death after permanent prostate brachytherapy. Int J Radiat Oncol Biol Phys 2008;72:433-40.  |
| 39. | Aveyard P, Adab P, Cheng KK, Wallace DM, Hey K, Murphy MF. Does smoking status influence the prognosis of bladder cancer? A systematic review. BJU Int 2002;90:228-39.  |
| 40. | Kenfield SA, Stampfer MJ, Chan JM, Giovannucci E. Smoking and prostate cancer survival and recurrence. JAMA 2011;305:2548-55.  |
| 41. | Richardson GE, Tucker MA, Venzon DJ, Linnoila RI, Phelps R, Phares JC, et al. Smoking cessation after successful treatment of small-cell lung cancer is associated with fewer smoking-related second primary cancers. Ann Intern Med 1993;119:383-90.  |
| 42. | Gillison ML, Zhang Q, Jordan R, Xiao W, Westra WH, Trotti A, et al. Tobacco smoking and increased risk of death and progression for patients with p16-positive and p16-negative oropharyngeal cancer. J Clin Oncol 2012;30:2102-11.  |
| 43. | American Society of Clinical Oncology. American Society of Clinical Oncology policy statement update: Tobacco control – Reducing cancer incidence and saving lives. 2003. J Clin Oncol 2003;21:2777-86.  |
| 44. | Viswanath K, Herbst RS, Land SR, Leischow SJ, Shields PG, Writing Committee for the AACR Task Force on Tobacco and Cancer. Tobacco and cancer: An American Association for Cancer Research policy statement. Cancer Res 2010;70:3419-30.  |
| 45. | Available from: http://www.nccn.org. [Last accessed 2012 Dec 26].  |
| 46. | Fiore MC, Jaen CR, Baker TB, et al. Treating Tobacco Use and Dependence: 2008 Update. Clinical Practice Guideline. Rockville, MD: U.S. Department of Health and Human Services. Public Health Service. May 2008.  |
| 47. | Benowitz NL. Neurobiology of nicotine addiction: Implications for smoking cessation treatment. Am J Med 2008;121:S3-10.  |
| 48. | Hukkanen J, Jacob P 3 rd , Benowitz NL. Metabolism and disposition kinetics of nicotine. Pharmacol Rev 2005;57:79-115.  |
| 49. | Tutka P, Mosiewicz J, Wielosz M. Pharmacokinetics and metabolism of nicotine. Pharmacol Rep 2005;57:143-53.  |
| 50. | Shields PG. Epidemiology of tobacco carcinogenesis. Curr Oncol Rep 2000;2:257-62.  |
| 51. | Dennis PA, Van Waes C, Gutkind JS, Kellar KJ, Vinson C, Mukhin AG, et al. The biology of tobacco and nicotine: Bench to bedside. Cancer Epidemiol Biomarkers Prev 2005;14:764-7.  |
| 52. | Singh S, Pillai S, Chellappan S. Nicotinic acetylcholine receptor signaling in tumor growth and metastasis. J Oncol 2011;2011:456743.  |
| 53. | Schuller HM. Regulatory role of the α7nAChR in cancer. Curr Drug Targets 2012;13:680-7.  |
| 54. | Schuller HM, Porter B, Riechert A. Beta-adrenergic modulation of NNK-induced lung carcinogenesis in hamsters. J Cancer Res Clin Oncol 2000;126:624-30.  |
| 55. | Rioux N, Castonguay A. Inhibitors of lipoxygenase: A new class of cancer chemopreventive agents. Carcinogenesis 1998;19:1393-400.  |
| 56. | Rioux N, Castonguay A. Prevention of NNK-induced lung tumorigenesis in A/J mice by acetylsalicylic acid and NS-398. Cancer Res 1998;58:5354-60.  |
| 57. | Schuller HM. Mechanisms of smoking-related lung and pancreatic adenocarcinoma development. Nat Rev Cancer 2002;2:455-63.  |
| 58. | Arredondo J, Chernyavsky AI, Grando SA. Nicotinic receptors mediate tumorigenic action of tobacco-derived nitrosamines on immortalized oral epithelial cells. Cancer Biol Ther 2006;5:511-7.  |
| 59. | Paleari L, Sessa F, Catassi A, Servent D, Mourier G, Doria-Miglietta G, et al. Inhibition of non-neuronal alpha7-nicotinic receptor reduces tumorigenicity in A549 NSCLC xenografts. Int J Cancer 2009;125:199-211.  |
| 60. | Tsai JR, Chong IW, Chen CC, Lin SR, Sheu CC, Hwang JJ. Mitogen-activated protein kinase pathway was significantly activated in human bronchial epithelial cells by nicotine. DNA Cell Biol 2006;25:312-22.  |
| 61. | Soma T, Kaganoi J, Kawabe A, Kondo K, Imamura M, Shimada Y. Nicotine induces the fragile histidine triad methylation in human esophageal squamous epithelial cells. Int J Cancer 2006;119:1023-7.  |
| 62. | Nakada T, Kiyotani K, Iwano S, Uno T, Yokohira M, Yamakawa K, et al. Lung tumorigenesis promoted by anti-apoptotic effects of cotinine, a nicotine metabolite through activation of PI3K/Akt pathway. J Toxicol Sci 2012;37:555-63.  |
| 63. | Maier CR, Hollander MC, Hobbs EA, Dogan I, Linnoila RI, Dennis PA. Nicotine does not enhance tumorigenesis in mutant K-ras-driven mouse models of lung cancer. Cancer Prev Res (Phila) 2011;4:1743-51.  |
| 64. | Murphy SE, von Weymarn LB, Schutten MM, Kassie F, Modiano JF. Chronic nicotine consumption does not influence 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone-induced lung tumorigenesis. Cancer Prev Res (Phila) 2011;4:1752-60.  |
| 65. | Guo J, Chu M, Abbeyquaye T, Chen CY. Persistent nicotine treatment potentiates amplification of the dihydrofolate reductase gene in rat lung epithelial cells as a consequence of ras activation. J Biol Chem 2005;280:30422-31.  |
| 66. | Chu M, Guo J, Chen CY. Long-term exposure to nicotine, via ras pathway, induces cyclin D1 to stimulate G1 cell cycle transition. J Biol Chem 2005;280:6369-79.  |
| 67. | Puliyappadamba VT, Cheriyan VT, Thulasidasan AK, Bava SV, Vinod BS, Prabhu PR, et al. Nicotine-induced survival signaling in lung cancer cells is dependent on their p53 status while its down-regulation by curcumin is independent. Mol Cancer 2010;9:220.  |
| 68. | Nishioka T, Yamamoto D, Zhu T, Guo J, Kim SH, Chen CY. Nicotine overrides DNA damage-induced G1/S restriction in lung cells. PLoS One 2011;6:e18619.  |
| 69. | Jorgensen ED, Zhao H, Traganos F, Albino AP, Darzynkiewicz Z. DNA damage response induced by exposure of human lung adenocarcinoma cells to smoke from tobacco- and nicotine-free cigarettes. Cell Cycle 2010;9:2170-6.  |
| 70. | Murray RP, Connett JE, Zapawa LM. Does nicotine replacement therapy cause cancer? Evidence from the Lung Health Study. Nicotine Tob Res 2009;11:1076-82.  |
| 71. | Zhu BQ, Heeschen C, Sievers RE, Karliner JS, Parmley WW, Glantz SA, et al. Second hand smoke stimulates tumor angiogenesis and growth. Cancer Cell 2003;4:191-6.  |
| 72. | Song P, Sekhon HS, Jia Y, Keller JA, Blusztajn JK, Mark GP, et al. Acetylcholine is synthesized by and acts as an autocrine growth factor for small cell lung carcinoma. Cancer Res 2003;63:214-21.  |
| 73. | Quik M, Chan J, Patrick J. alpha-Bungarotoxin blocks the nicotinic receptor mediated increase in cell number in a neuroendocrine cell line. Brain Res 1994;655:161-7.  |
| 74. | Fucile S, Napolitano M, Mattei E. Cholinergic stimulation of human microcytoma cell line H69. Biochem Biophys Res Commun 1997;230:501-4.  |
| 75. | Novak J, Escobedo-Morse A, Kelley K, Boose D, Kautzman-Eades D, Meyer M, et al. Nicotine effects on proliferation and the bombesin-like peptide autocrine system in human small cell lung carcinoma SHP77 cells in culture. Lung Cancer 2000;29:1-10.  |
| 76. | Arredondo J, Chernyavsky AI, Grando SA. The nicotinic receptor antagonists abolish pathobiologic effects of tobacco-derived nitrosamines on BEP2D cells. J Cancer Res Clin Oncol 2006;132:653-63.  |
| 77. | Schuller HM. Cell type specific, receptor-mediated modulation of growth kinetics in human lung cancer cell lines by nicotine and tobacco-related nitrosamines. Biochem Pharmacol 1989;38:3439-42.  |
| 78. | Codignola A, Tarroni P, Cattaneo MG, Vicentini LM, Clementi F, Sher E. Serotonin release and cell proliferation are under the control of alpha-bungarotoxin-sensitive nicotinic receptors in small-cell lung carcinoma cell lines. FEBS Lett 1994;342:286-90.  |
| 79. | Cattaneo MG, Codignola A, Vicentini LM, Clementi F, Sher E. Nicotine stimulates a serotonergic autocrine loop in human small-cell lung carcinoma. Cancer Res 1993;53:5566-8.  |
| 80. | Al-Wadei MH, Al-Wadei HA, Schuller HM. Pancreatic cancer cells and normal pancreatic duct epithelial cells express an autocrine catecholamine loop that is activated by nicotinic acetylcholine receptors α3, α5, and α7. Mol Cancer Res 2012;10:239-49.  |
| 81. | Trombino S, Cesario A, Margaritora S, Granone P, Motta G, Falugi C, et al. Alpha7-nicotinic acetylcholine receptors affect growth regulation of human mesothelioma cells: Role of mitogen-activated protein kinase pathway. Cancer Res 2004;64:135-45.  |
| 82. | Shin VY, Wu WK, Chu KM, Wong HP, Lam EK, Tai EK, et al. Nicotine induces cyclooxygenase-2 and vascular endothelial growth factor receptor-2 in association with tumor-associated invasion and angiogenesis in gastric cancer. Mol Cancer Res 2005;3:607-15.  |
| 83. | Shin VY, Wu WK, Ye YN, So WH, Koo MW, Liu ES, et al. Nicotine promotes gastric tumor growth and neovascularization by activating extracellular signal-regulated kinase and cyclooxygenase-2. Carcinogenesis 2004;25:2487-95.  |
| 84. | Ye YN, Liu ES, Shin VY, Wu WK, Luo JC, Cho CH. Nicotine promoted colon cancer growth via epidermal growth factor receptor, c-Src, and 5-lipoxygenase-mediated signal pathway. J Pharmacol Exp Ther 2004;308:66-72.  |
| 85. | Dasgupta P, Rastogi S, Pillai S, Ordonez-Ercan D, Morris M, Haura E, et al. Nicotine induces cell proliferation by beta-arrestin-mediated activation of Src and Rb-Raf-1 pathways. J Clin Invest 2006;116:2208-2217.  |
| 86. | Chini B, Clementi F, Hukovic N, Sher E. Neuronal-type alpha-bungarotoxin receptors and the alpha 5-nicotinic receptor subunit gene are expressed in neuronal and nonneuronal human cell lines. Proc Natl Acad Sci U S A 1992;89:1572-6.  |
| 87. | Ye YN, Liu ES, Shin VY, Wu WK, Cho CH. The modulating role of nuclear factor-kappaB in the action of alpha7-nicotinic acetylcholine receptor and cross-talk between 5-lipoxygenase and cyclooxygenase-2 in colon cancer growth induced by 4-(N-methyl-N-nitrosamino)-1-(3-pyridyl)-1-butanone. J Pharmacol Exp Ther 2004;311:123-30.  |
| 88. | Tsurutani J, Castillo SS, Brognard J, Granville CA, Zhang C, Gills JJ, et al. Tobacco components stimulate Akt-dependent proliferation and NFkappaB-dependent survival in lung cancer cells. Carcinogenesis 2005;26:1182-95.  |
| 89. | Askari MD, Tsao MS, Schuller HM. The tobacco-specific carcinogen, 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone stimulates proliferation of immortalized human pancreatic duct epithelia through beta-adrenergic transactivation of EGF receptors. J Cancer Res Clin Oncol 2005;131:639-48.  |
| 90. | Jin Z, Gao F, Flagg T, Deng X. Tobacco-specific nitrosamine 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone promotes functional cooperation of Bcl2 and c-Myc through phosphorylation in regulating cell survival and proliferation. J Biol Chem 2004;279:40209-19.  |
| 91. | Heeschen C, Jang JJ, Weis M, Pathak A, Kaji S, Hu RS, et al. Nicotine stimulates angiogenesis and promotes tumor growth and atherosclerosis. Nat Med 2001;7:833-9.  |
| 92. | Heeschen C, Weis M, Aicher A, Dimmeler S, Cooke JP. A novel angiogenic pathway mediated by non-neuronal nicotinic acetylcholine receptors. J Clin Invest 2002;110:527-36.  |
| 93. | Brown KC, Lau JK, Dom AM, Witte TR, Luo H, Crabtree CM, et al. MG624, an α7-nAChR antagonist, inhibits angiogenesis via the Egr-1/FGF2 pathway. Angiogenesis 2012;15:99-114.  |
| 94. | Shin VY, Jin HC, Ng EK, Cho CH, Leung WK, Sung JJ, et al. 4-(Methylnitrosamino)-1-(3-pyridyl)-1-butanone promoted gastric cancer growth through prostaglandin E receptor (EP2 and EP4) in vivo and in vitro. Cancer Sci 2011;102:926-33.  |
| 95. | Jarzynka MJ, Guo P, Bar-Joseph I, Hu B, Cheng SY. Estradiol and nicotine exposure enhances A549 bronchioloalveolar carcinoma xenograft growth in mice through the stimulation of angiogenesis. Int J Oncol 2006;28:337-44.  |
| 96. | Dasgupta P, Chellappan SP. Nicotine-mediated cell proliferation and angiogenesis: New twists to an old story. Cell Cycle 2006;5:2324-8.  |
| 97. | Xu L, Deng X. Protein kinase Ciota promotes nicotine-induced migration and invasion of cancer cells via phosphorylation of micro- and m-calpains. J Biol Chem 2006;281:4457-66.  |
| 98. | Momi N, Ponnusamy MP, Kaur S, Rachagani S, Kunigal SS, Chellappan S, et al. Nicotine/cigarette smoke promotes metastasis of pancreatic cancer through α7nAChR-mediated MUC4 upregulation. Oncogene 2012;[Epub ahead of print].  |
| 99. | Kunigal S, Ponnusamy MP, Momi N, Batra SK, Chellappan SP. Nicotine, IFN-g and retinoic acid mediated induction of MUC4 in pancreatic cancer requires E2F1 and STAT-1 transcription factors and utilize different signaling cascades. Mol Cancer 2012;11:24.  |
| 100. | Lien YC, Wang W, Kuo LJ, Liu JJ, Wei PL, Ho YS, et al. Nicotine promotes cell migration through alpha7 nicotinic acetylcholine receptor in gastric cancer cells. Ann Surg Oncol 2011;18:2671-9.  |
| 101. | Wei PL, Kuo LJ, Huang MT, Ting WC, Ho YS, Wang W, et al. Nicotine enhances colon cancer cell migration by induction of fibronectin. Ann Surg Oncol 2011;18:1782-90.  |
| 102. | Pillai S, Rizwani W, Li X, Rawal B, Nair S, Schell MJ, et al. ID1 facilitates the growth and metastasis of non-small cell lung cancer in response to nicotinic acetylcholine receptor and epidermal growth factor receptor signaling. Mol Cell Biol 2011;31:3052-67.  |
| 103. | Xu L, Deng X. Tobacco-specific nitrosamine 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone induces phosphorylation of mu- and m-calpain in association with increased secretion, cell migration, and invasion. J Biol Chem 2004;279:53683-90.  |
| 104. | Shen J, Xu L, Owonikoko TK, Sun SY, Khuri FR, Curran WJ, et al. NNK promotes migration and invasion of lung cancer cells through activation of c-Src/PKCi/FAK loop. Cancer Lett 2012;318:106-13.  |
| 105. | Razani-Boroujerdi S, Singh SP, Knall C, Hahn FF, Peña-Philippides JC, Kalra R, et al. Chronic nicotine inhibits inflammation and promotes influenza infection. Cell Immunol 2004;230:1-9.  |
| 106. | Dasgupta P, Rizwani W, Pillai S, Kinkade R, Kovacs M, Rastogi S, et al. Nicotine induces cell proliferation, invasion and epithelial-mesenchymal transition in a variety of human cancer cell lines. Int J Cancer 2009;124:36-45.  |
| 107. | Hirata N, Sekino Y, Kanda Y. Nicotine increases cancer stem cell population in MCF-7 cells. Biochem Biophys Res Commun 2010;403:138-43.  |
| 108. | Dasgupta P, Kinkade R, Joshi B, Decook C, Haura E, Chellappan S. Nicotine inhibits apoptosis induced by chemotherapeutic drugs by up-regulating XIAP and survivin. Proc Natl Acad Sci U S A 2006;103:6332-7.  |
| 109. | Xin M, Deng X. Protein phosphatase 2A enhances the proapoptotic function of Bax through dephosphorylation. J Biol Chem 2006;281:18859-67.  |
| 110. | Zhang T, Lu H, Shang X, Tian Y, Zheng C, Wang S, et al. Nicotine prevents the apoptosis induced by menadione in human lung cancer cells. Biochem Biophys Res Commun 2006;342:928-34.  |
| 111. | Xin M, Deng X. Nicotine inactivation of the proapoptotic function of Bax through phosphorylation. J Biol Chem 2005;280:10781-9.  |
| 112. | Jin Z, Gao F, Flagg T, Deng X. Nicotine induces multi-site phosphorylation of Bad in association with suppression of apoptosis. J Biol Chem 2004;279:23837-44.  |
| 113. | Onoda N, Nehmi A, Weiner D, Mujumdar S, Christen R, Los G. Nicotine affects the signaling of the death pathway, reducing the response of head and neck cancer cell lines to DNA damaging agents. Head Neck 2001;23:860-70.  |
| 114. | Nishioka T, Guo J, Yamamoto D, Chen L, Huppi P, Chen CY. Nicotine, through upregulating pro-survival signaling, cooperates with NNK to promote transformation. J Cell Biochem 2010;109:152-61.  |
| 115. | Jin Z, Xin M, Deng X. Survival function of protein kinase C {iota} as a novel nitrosamine 4-(methylnitrosamino)-1-(3-pyridyl)-1-butanone-activated bad kinase. J Biol Chem 2005;280:16045-52.  |
| 116. | Warren GW, Romano MA, Kudrimoti MR, Randall ME, McGarry RC, Singh AK, et al. Nicotinic modulation of therapeutic response in vitro and in vivo. Int J Cancer 2012;131:2519-27.  |
Authors
Dr. Graham W. Warren, Departments of Radiation Medicine, and Pharmacology and Therapeutics, Roswell Park Cancer Institute, Buffalo, New York, USA
Dr. Anurag K. Singh, Department of Radiation Medicine, Roswell Park Cancer Institute, Buffalo, New York, USA
Figures
[Figure 1], [Figure 2]
